Dr Minh Alexander retired consultant psychiatrist 20 August 2022
We have a perfect storm of collapsed emergency services. Years of under investment in the NHS and social care, loss of safe capacity, bed cutting, delayed discharges, loss of NHS staff from Brexit, a pandemic that has been allowed to run wild and wreak havoc, COVID related NHS staff sickness, and dangerous waiting lists. Not a storm, a tsunami.
A data release of 11 August 2022 showed that NHS ambulance services in England are not meeting standards for even the most serious emergencies such as Category 1 calls for scenarios such as cardiac arrest.
There are daily media reports of egregious cases of ambulance delay and ambulance queues outside our hospitals.
Research by the GMB union released in July 2022 has shown that a horrifying 35% of ambulance workers witnessed deaths due to ambulance delays.
This week it was announced that the government’s “independent” investigation into the deaths cover up scandal at North East Ambulance Service (NEAS) will be headed by Marianne Griffiths, a former NHS Chief Executive.
NHS England commissioned Griffiths to undertake the investigation.
This is a far cry from the public inquiry sought by whistleblowers and bereaved families. Especially considering that NHS England has been criticised for failure to act on NEAS whistleblowers’ disclosures, and therefor has a conflict of interest in this matter.
Nevertheless, it is useful for context to this investigation to glance at relevant indicators that may shed light on NEAS’ workforce practices and governance.
Firstly, NEAS has been caught out trying to silence whistleblowers with highly inappropriate and unlawful secrecy clauses, to prevent them from pursuing public interest disclosures and requiring them to destroy evidence of wrongdoing.
NEAS’ past FOI disclosures and other information show following outlay on settlement agreements:
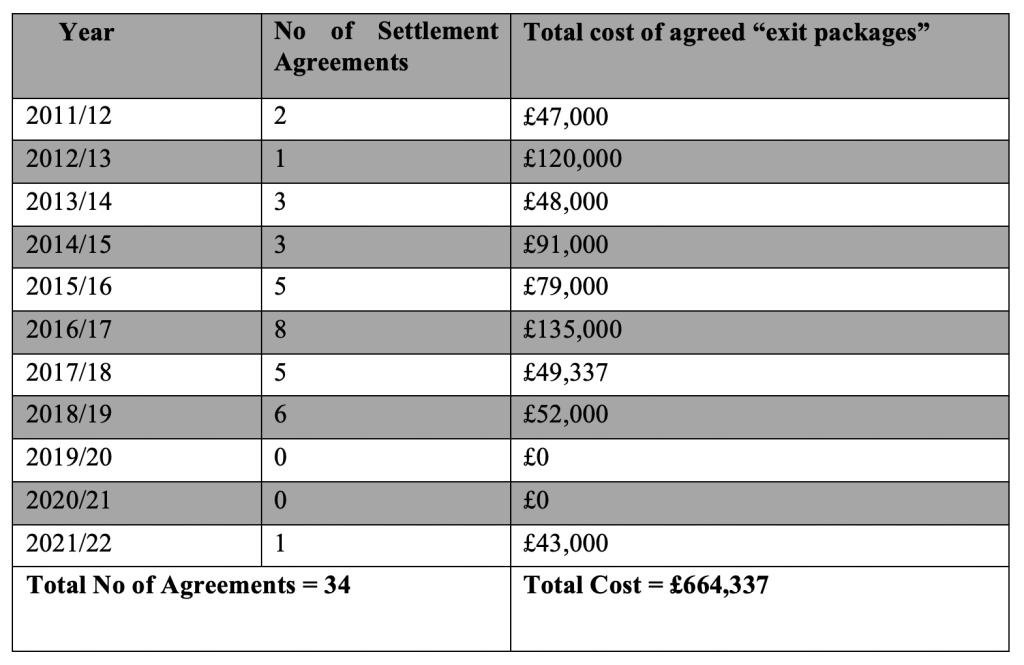
The settlement in 2021/22 is of special interest given what is known about the trust’s attempts to silence whistleblowers in the current deaths scandal, and the timeline of the scandal.
There are roughly 20,000 ambulance trust staff.
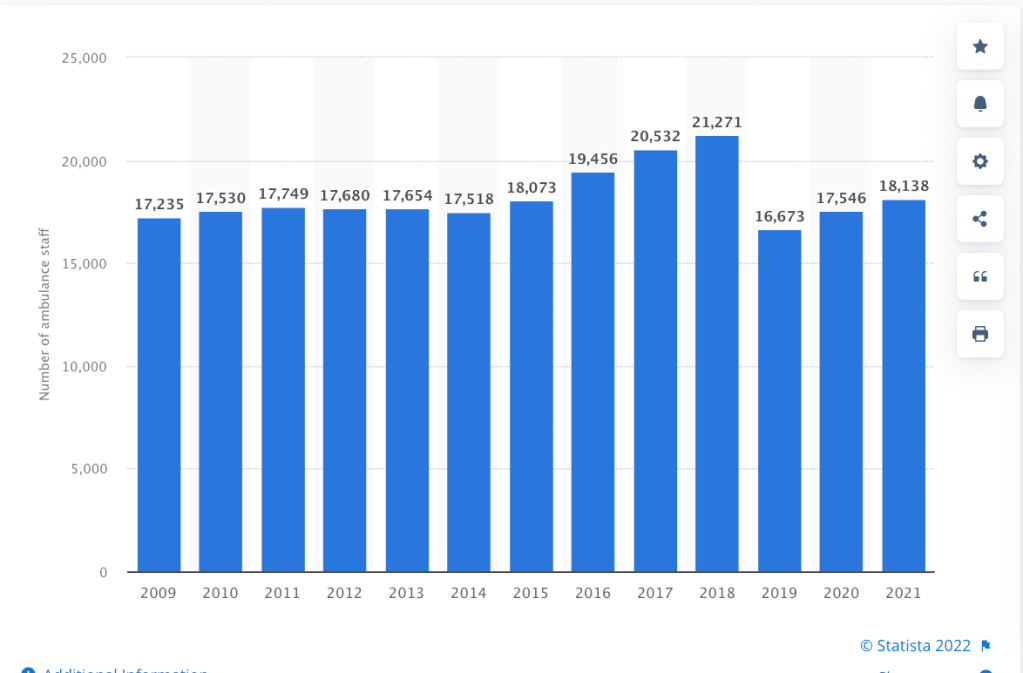
Based on NHS Digital data, NEAS has a trend towards increasing numbers of staff leaving in recent years. It shares this in common with other ambulance trusts.
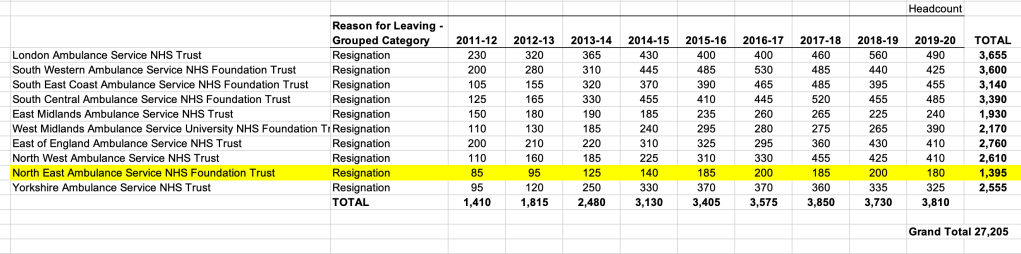
Between 2011 and 2019, 1,395 NEAS staff resigned. The trust’s establishment is about 3,000 staff.
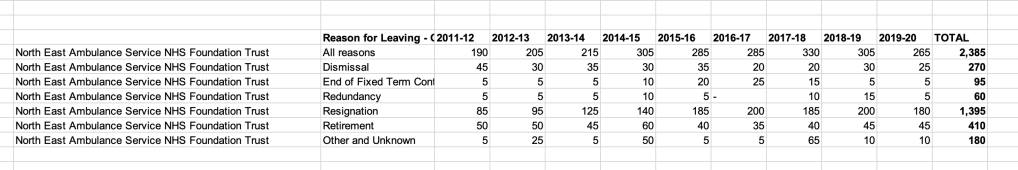
Between 2011 and 2019, a total of 42,350 NHS ambulance trust staff in England left:
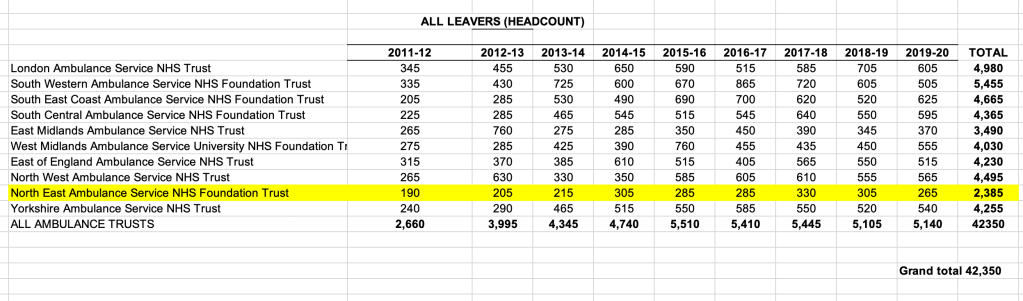
Between 2011 and 2019 a total of 27,205 NHS ambulance trust staff in England resigned:
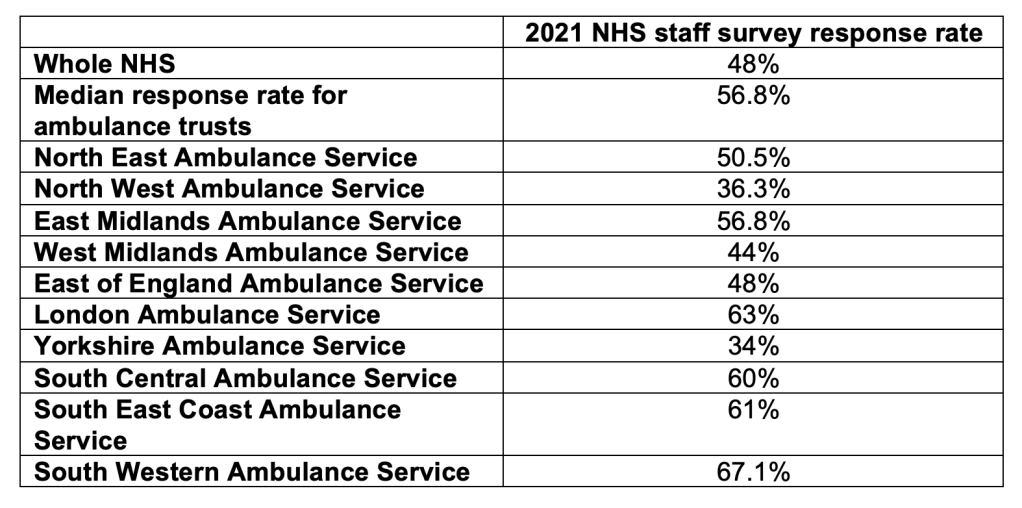
The NHS staff survey is another source of data on workforce relations. The overall response rate for the NHS is poor. Amongst ambulance trusts there is great variation in the response rate, raising some questions about the validity of the data and staff engagement in some of the trusts. Alternatively, it may also reflect the management approach to staff “compliance” with the survey:
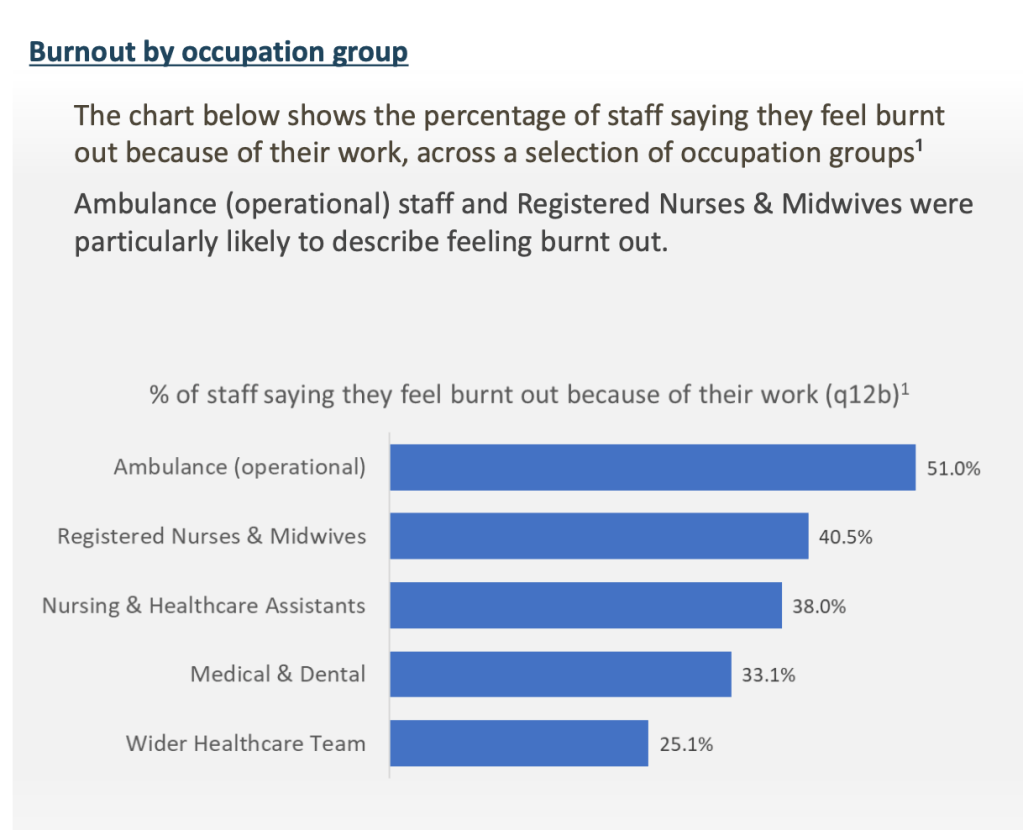
The 2021 NHS staff survey confirmed that ambulance trust operational staff experience the highest levels of burnout:
At present, about one in ten NHS posts are vacant.
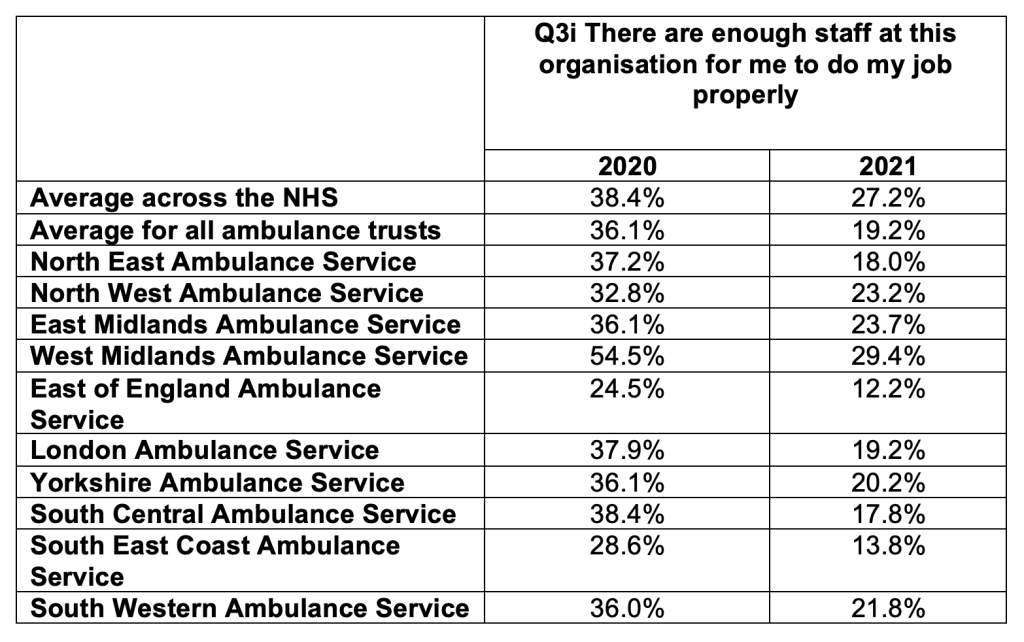
The 2021 NHS staff survey revealed that ambulance staff are the group most likely to report detrimental understaffing:
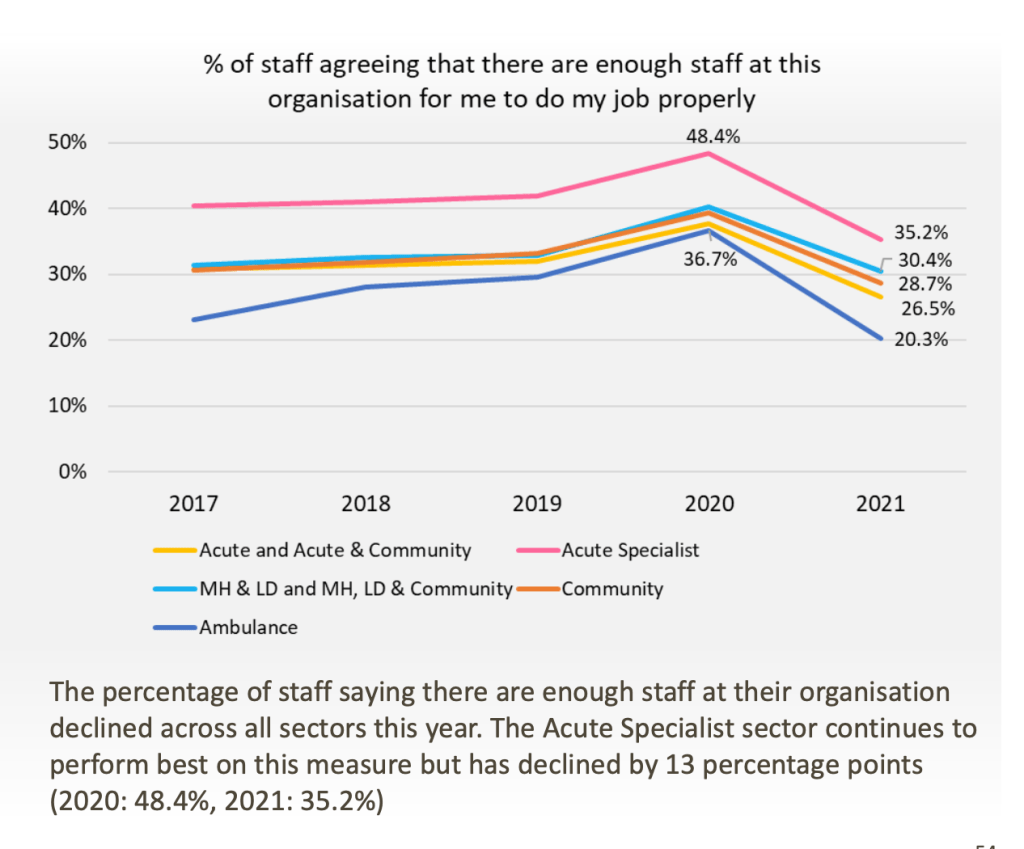
This table shows how this metric on the NHS staff survey plummeted at ambulance trusts between 2020 and 2021. The most shockingly low score was at East of England Ambulance Service, where only 12.2% of staff thought there was sufficient staffing:
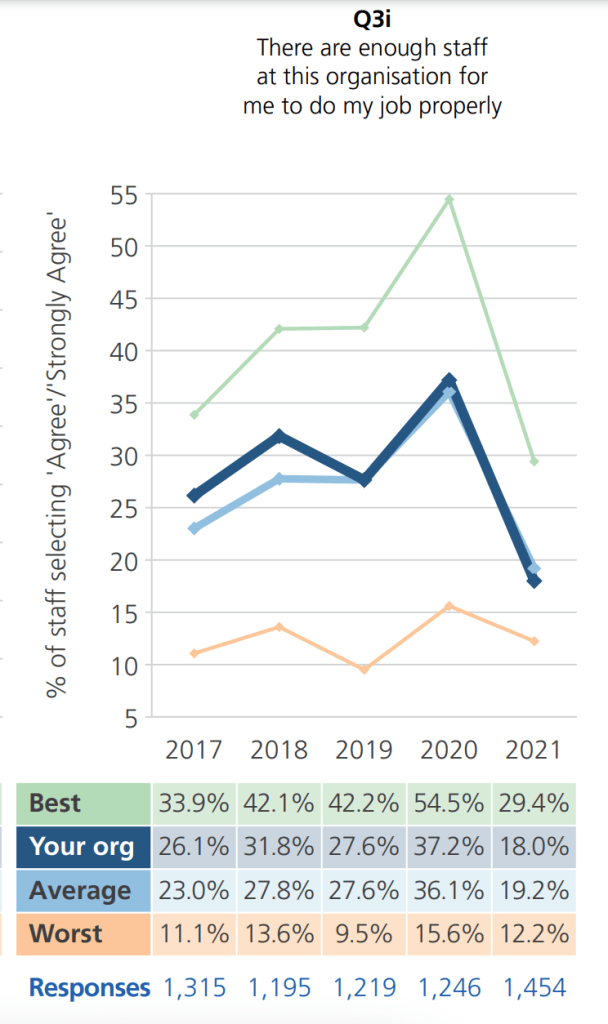
In recent years, roughly only a quarter of NEAS staff thought that there was safe staffing:
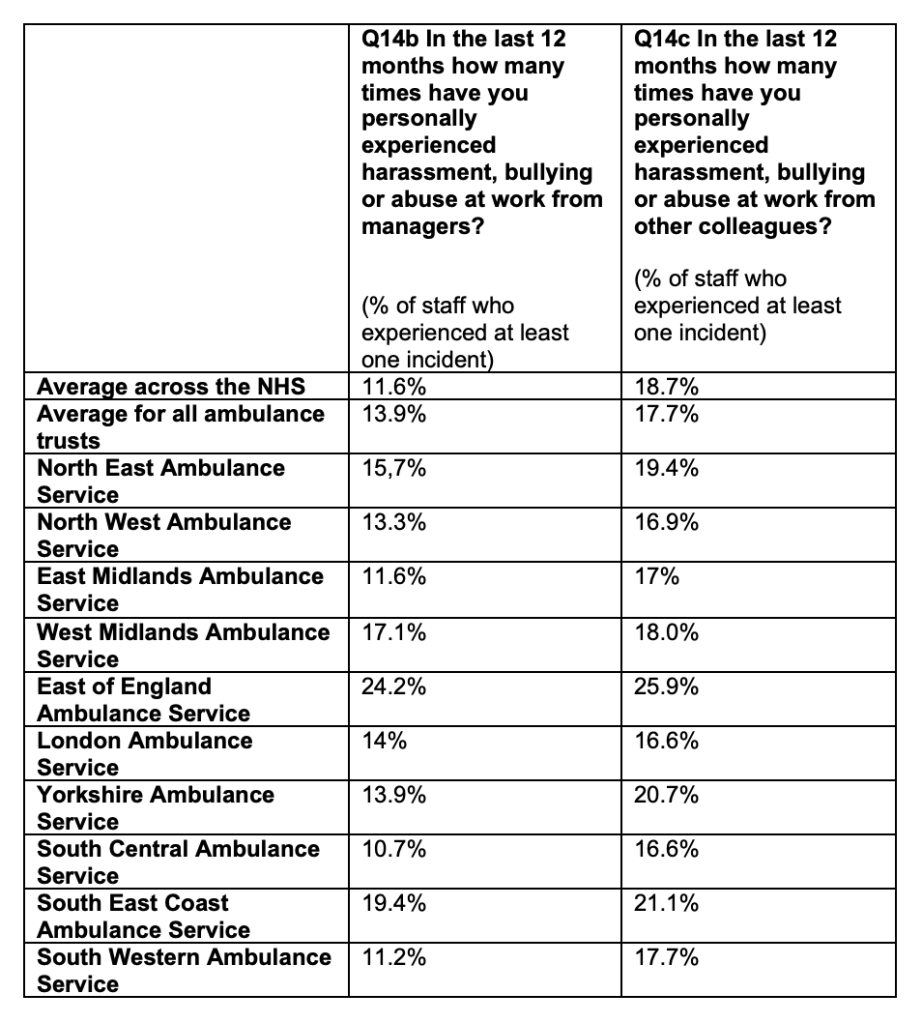
Ambulance trusts used to be gross outliers for bullying. This has improved in recent years, but most ambulance trusts still have levels of bullying above the national average. East of England Ambulance Service remains a gross outlier. This was the rate of reported bullying for each ambulance trust in 2021:
Ambulance trust staff gave mixed messages on the 2021 staff survey questions about whistleblowing, in common with the rest of the NHS. There is higher scoring on feeling able to report unsafe care, but a decrease in the perception that staff can speak out about anything. As has consistently been the case, staff are less likely to think that concerns will be addressed:
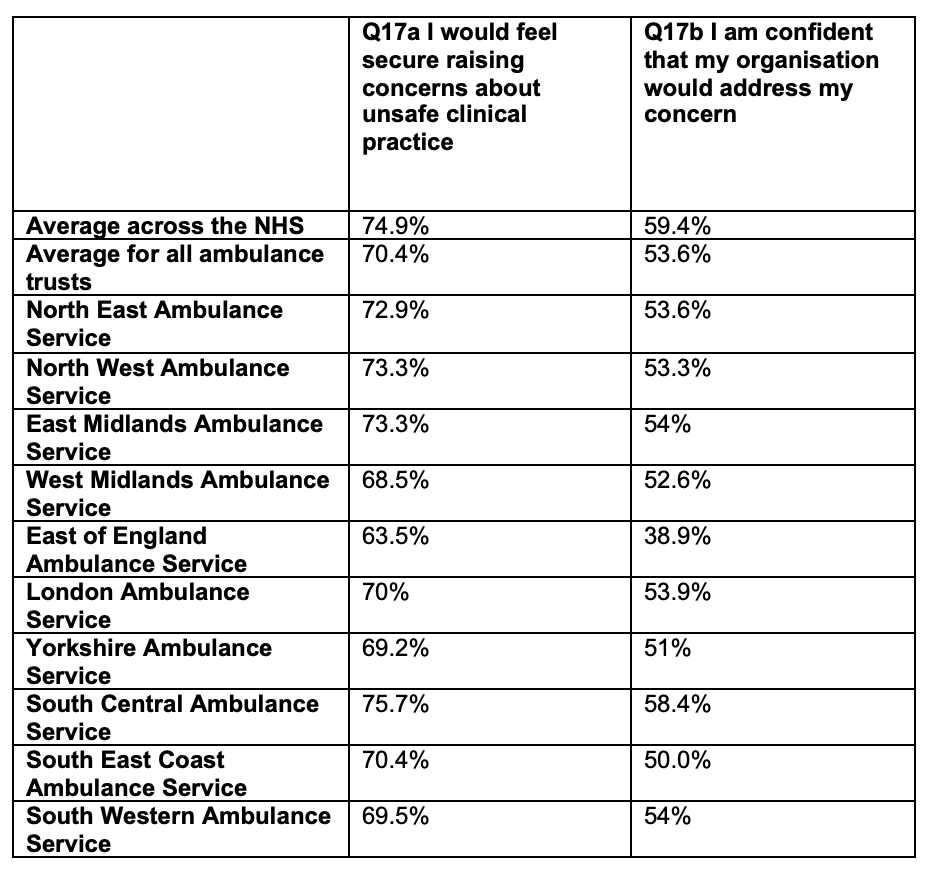
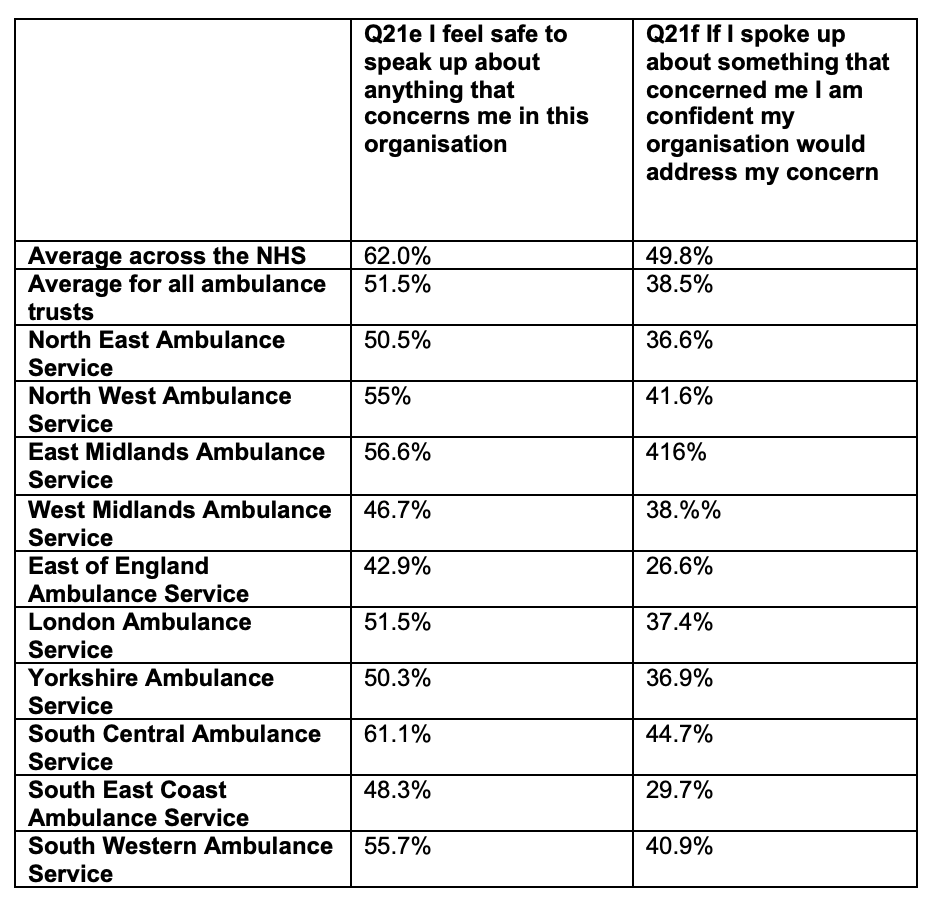
The above are hypothetical questions about what might happen.
On a question about what actually happened, Ambulance trust staff said they under-reported bullying to the following degrees, which raises questions of engagement and trust. Ambulance trusts are all below the national NHS average for reporting bullying:
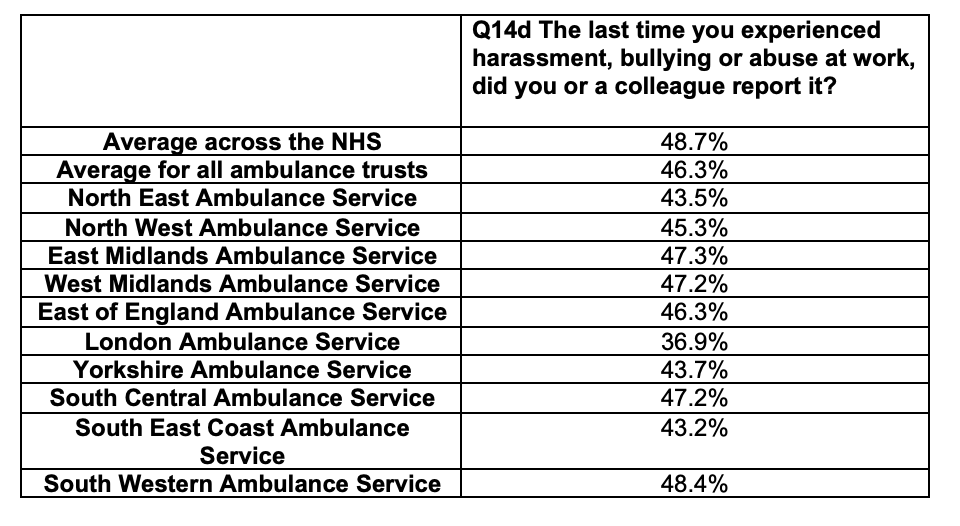
But that might not be so surprising given that the NHS staff survey composite scores on “compassionate leadership” is the lowest overall for ambulance trusts:
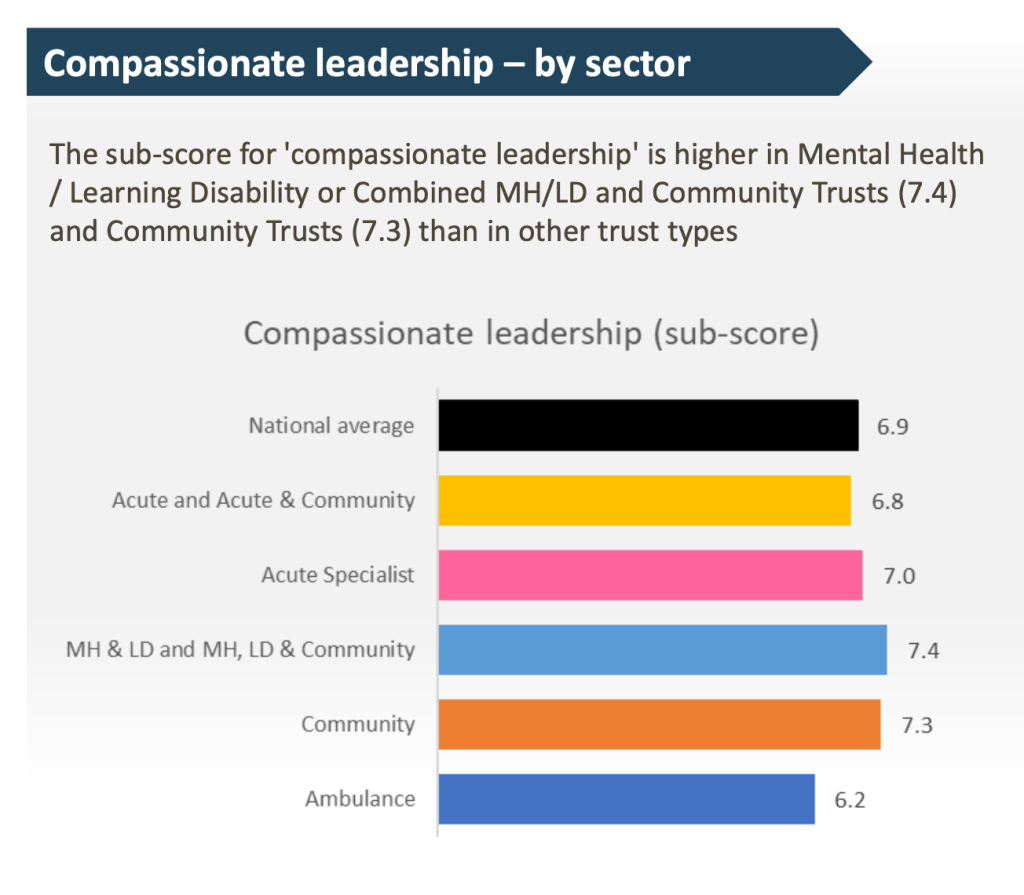
We shall see how the Dame handles the deaths scandal at NEAS.
It is worth bearing in mind that she had a whistleblowing scandal of her own, which the former National Freedom To Speak Up Guardian helped to suppress by breaching her own procedures in a most arbitrary and extraordinary way:
A Study in Delay: The National Guardian & Brighton and Sussex University Hospitals NHS Trust
As often happens when you sweep dirt under the carpet, it contributed to a patient safety mess later on:
PETITION
Please click and add your signature to this petition to reform UK whistleblowing
law – whistleblowers protect us all but weak UK law leaves them wholly exposed,
lets abusers off the hook and it is a threat to public safety.
Replace weak UK
whistleblowing law and protect whistleblowers and the public
RELATED ITEMS
Staff suicides at West Midlands Ambulance Service NHS Foundation Trust
The National Guardian’s Office does not put a blue light on for ambulance staff


