By Dr Minh Alexander retired consultant psychiatrist 11 June 2022
This is a post to share data. It follows the trail of press reports of whistleblowing at HSIB and the King’s Fund review into culture and leadership at the troubled Healthcare Safety Investigation Branch (HSIB). This review raised particular issues of poor management in some of the regional maternity teams.
Information was requested from HSIB about “letters of concern” sent by HSIB to NHS trusts with particularly serious maternity safety failings and related poor governance.
Information was also requested on any evidence of conflicts of interest in HSIB’s own maternity operations, particularly in the light of the King’s Funds findings of HSIB staff perception of “unfairness” and “favouritism”.
| HSIB’s maternity investigation function and conflicts of interest In 2017 Jeremy Hunt the then Health Secretary caused consternation by announcing that the tiny and recently formed HSIB which was originally intended to undertake 30 nationally relevant investigations a year should rapidly expand to undertake a thousand maternity investigations as well. The maternity programme became operational in 2018. The central HSIB team investigated cases of national relevance under ‘safe space’ provisions. In contrast, there were fourteen regional maternity HSIB teams with links to each trust providing maternity services, which investigated individual cases but not under ‘safe space’ provisions. Concerns had been raised that applying ‘safe space’ to the local HSIB maternity investigations would obstruct duty of candour. A government proposal to allow some “accredited” NHS trusts to run their own safe space investigations in due course was kicked out entirely by parliament as “wholly misconceived” and unsafely riddled with conflict of interest. A less discussed issue is that of conflicts of interest arising from the local connections of HSIB maternity investigators. After the Midstaffs scandal, the Healthcare Commission – the regulator which exposed the scandal was scrapped and replaced with the much criticised Care Quality Commission. One of the first acts of the CQC was to disband a central investigation team and replace it with dispersed local teams and “relationship owners” assigned to individual provider organisations. This was criticised because of the increased risk of regulatory capture: “…regional officers are at risk of what she calls “regulatory capture”. They can become too close to the trust managers they are supposed to monitor – and too keen to see them succeed” It seems to me that the dispersed model of the HSIB maternity programme risks exactly the same type of capture. It also embeds conflicts of interest due to recruitment of maternity staff from the regions. Moreover, a 2020 internal report on HSIB’s maternity programme disclosed by NHSE/I noted significant cultural issues of bullying and problems with challenge and speaking up, and a chaotic lack of defined standards. The latter were attributed to the rapid expansion of the maternity programme, and could perhaps also be considered an artefact of the regionalisation of the service. |
NEW INFORMATION FROM HSIB
The latest data from HSIB has revealed that between 1st April 2018 and 31st March 2022, HSIB sent a total of 152 “letters of concern” to NHS trusts involved in the national maternity investigation programme.
These letters are sent when there is serious and urgent concern about patient safety:
“The urgent/emerging concerns panel will consider the significance and seriousness of the concerns raised and the urgency with which escalation should occur.
If outcome of urgent/emerging concerns panel is to proceed with escalation, then a letter detailing concerns is sent via email to the head of midwifery (HoM) or director of midwifery (DoM) and relevant clinical director (CD), and/or head of patient safety at the NHS trust.
The urgent/emerging concerns panel will decide if anyone else from the NHS trust should be copied into the escalation letter. Trust executives (medical director and chief nurse/DoM) copied into all escalation letters. Initial letters of escalation will be sent by RL [Regional Lead]/PNI [Principal National Investigator] unless panel consider otherwise.”
Depending on a trust’s response, HSIB has further stages of escalation, ending ultimately in onwards referral by HSIB’s Chief Investigator:
“HSIB chief investigator makes formal referral of concerns to CQC chief inspector of hospitals or referral to relevant professional regulator.”
The corollary of this seems to be that a dishonest but skilful trust could manipulate this escalation scheme by genuflecting and getting HSIB off its back with the right response, sincere or not.
Interestingly, HSIB has disclosed that it has no interagency protocols:
“We do not have any interagency protocols.”
This is HSIB’s escalation policy which determines the process for sending letters of concern to trusts:
HSIB Procedure for escalating significant safety concerns arising from investigations V3 2019
Some trusts have received no HSIB letters of concern, and one trust received 15 letters of concern, which was the highest number.
There are concerns from some bereaved families that some trusts which have so far escaped significant criticism and scrutiny in fact also have elevated levels of maternity serious incidents. This raises a question of whether some trusts have had an easier ride than is warranted.
An FOI disclosure by Maidstone and Wells NHS Trust of 22 September 2021 gives an example of the contents of an HSIB letter of concern:

HSIB volunteered undated spreadsheet data which goes up to 2021, which at that point showed a total of 29 letters of concern, sent to sixteen trusts.
Nottingham had been sent the most letters (five) at that point:
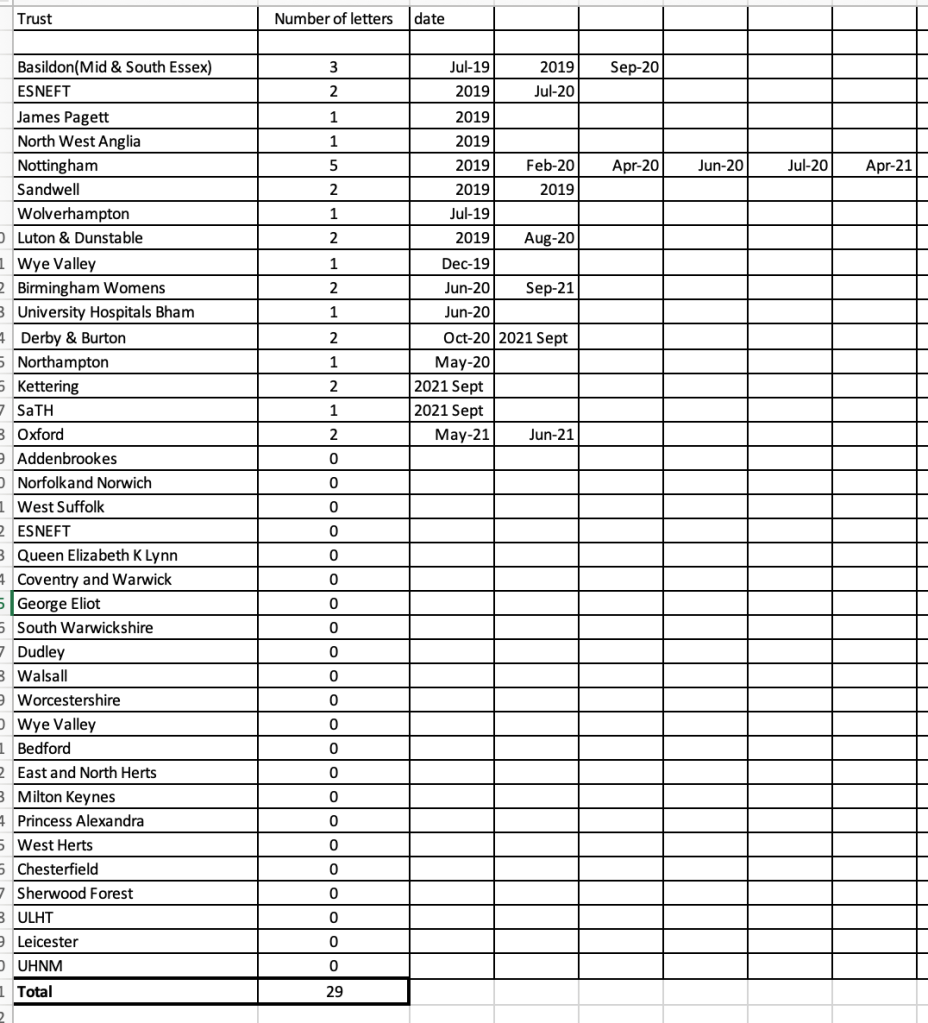
An up-to-date version of this spreadsheet has been requested, with breakdown of the number of letters of concern by trust.
So it would seem that there has been a huge acceleration in the number of HSIB escalation letters sent over the last year or so, jumping from a total of 29 to 152.
Does that have anything to do with the subsequent government announcement that HSIB will be stripped of its maternity investigations and that a short life special health authority under direct government control will be created, to replace the HSIB maternity investigation function?
As regards conflicts of interests in its regional maternity teams, HSIB maintains that it has these provisions in place to manage conflicts:
6. Please advise what due diligence NHSI undertook to ensure that appointments to regional HSIB maternity investigation teams were not compromised by conflicts of interest.
“NHS England and Improvement have not been involved, at any stage, in appointments or organising maternity teams. All maternity employees of HSIB are required to and have completed an annual declaration of interest form, highlighting trusts they have previously worked in or other known associated conflicts of interest. Maternity investigators do not carry out investigations in trusts they have previously worked in. Individuals are required to flag any conflicts of interest that may present during an investigation to enable them to be removed from the case, these may not relate to the trust.”
7. Please advise of HSIB’s approach to eliminating conflicts of interest in individual maternity investigations, by regional teams. Please disclose any relevant written guidance, policy or protocol.
“All maternity programme employees complete a declaration of interest form. Maternity investigators do not investigate in trusts they have previously worked in. Additionally, clinical advisors do not review or offer clinical advice in trusts they work in or have any associated conflicts of interest.”
But are these arrangements robust enough? It is not just individual HSIB investigators who matter, but their managers also impact on how investigations are handled and reported.
As an example, this is the CV of an HSIB Maternity investigation Team Leader according to her LinkedIn entry:
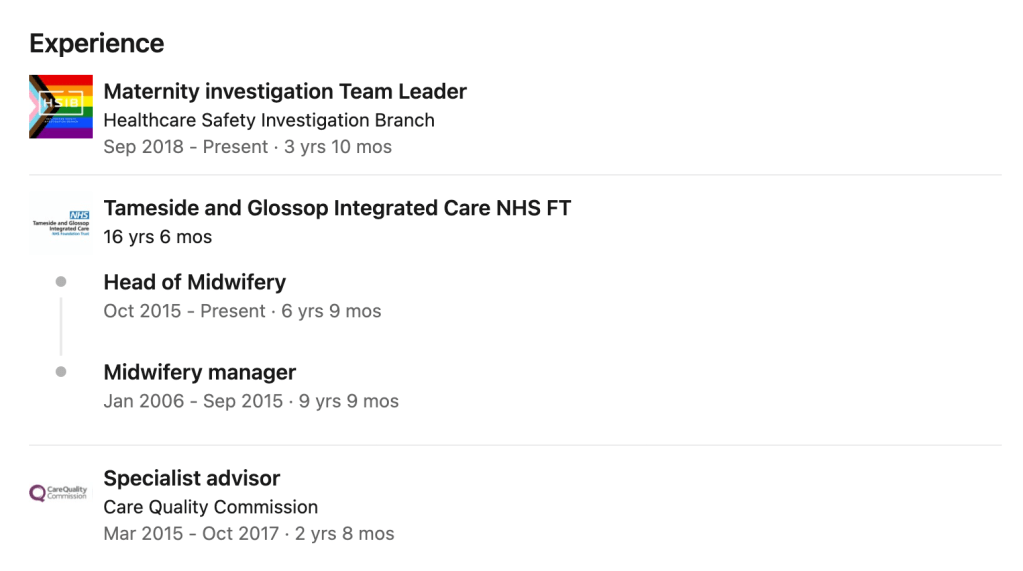
This is the CV of the HSIB Head of Maternity Investigations for HSIB according to her LinkedIn entry, who previously had a regional NHS England role in Midwifery:
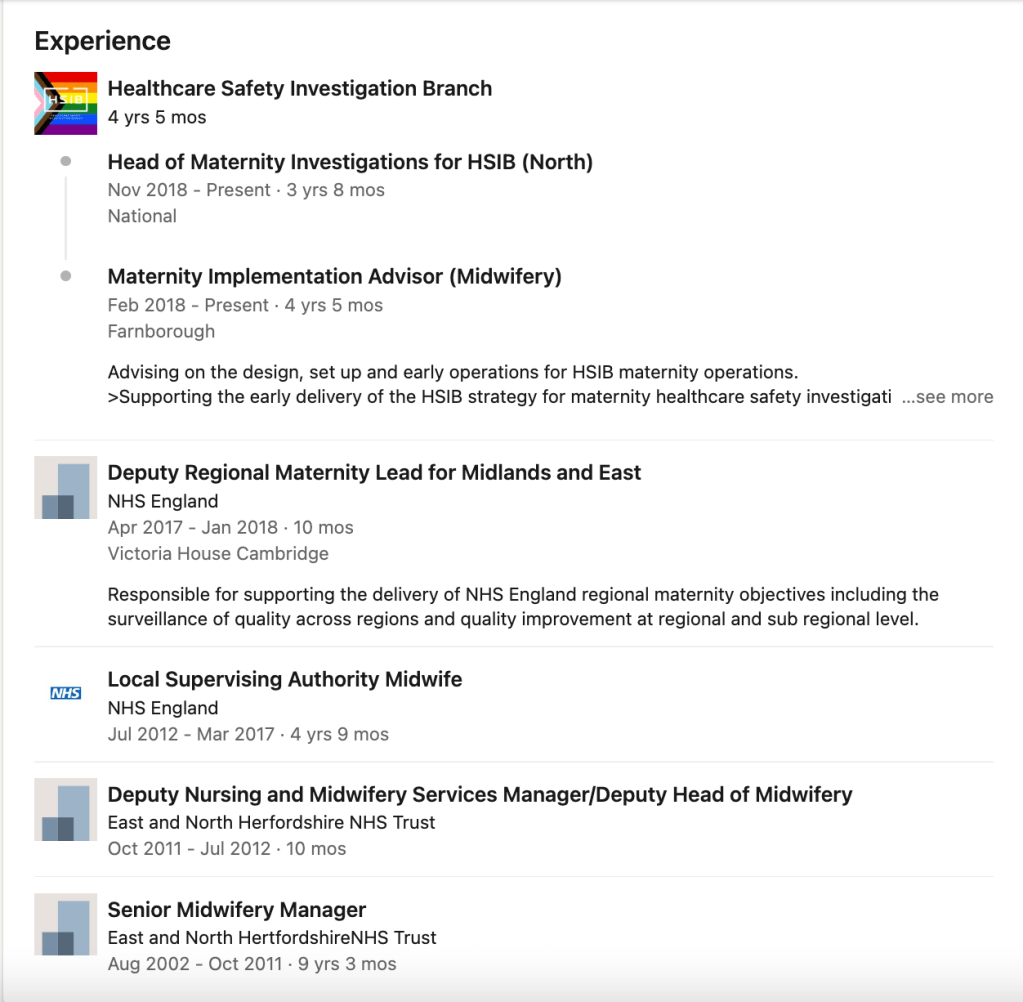
How do HSIB conflict of interest procedures apply to its regional maternity managers, especially those who have had past oversight of trusts in the same area/region?
Obviously, such individuals may potentially be conflicted in revealing evidence of past governance failure in their area/region.
When asked if there have been complaints or concerns about conflicts of interest, HSIB replied that there had been no complaints. It is less clear if there have been concerns eg. whistleblowing:
8. How many complaints and concerns has HSIB received about actual, potential or perceived conflicts of interest in maternity investigations by regional teams?”
“HSIB have received no complaints, that relate to actual, potential or perceived conflicts of interest relating to any part of the HSIB organisation.”
PETITION
Please click and add your signature to this petition to reform UK whistleblowing law – whistleblowers protect us all but weak UK law ignores their concerns, leaves them wholly exposed, lets abusers off the hook and it is a threat to public safety.
Replace weak UK whistleblowing law and protect whistleblowers and the public
RELATED ITEMS
What did Hunt do to the NHS – and how has he got away with it?

