By Dr Minh Alexander retired consultant psychiatrist 3 December 2022
For decades the UK Government has resisted good whistleblowing governance across all sectors. It has refused to meaningfully reform very weak UK whistleblowing law.
It hired lawyer Robert Francis to review whistleblowing in the NHS after the Mid Staffs scandal.
Despite recognising that UK whistleblowing law is weak, Francis declined to support legislative reform. He claimed in his 2015 review report that it would take too long, and that his go-faster model, the Freedom To Speak Up model, would be more expedient.
Later however, Francis claimed in 2020 correspondence that his model required time to work. A third party sent me correspondence from Francis, which stated:
14 January 2020:
“I fear we are not going to agree about the value of the Freedom to Speak Up National Guardian. Her office and the network she leads is making a great deal of progress on promoting the freedom to speak up without legislative or regulatory powers. The concept of guardians in this context is a new one and needs time to develop.”
Francis also claimed expansively in his 2015 review report that his model would make serious reprisal in the NHS “very rare”. Possibly a claim that he now rues, given the steady stream of suspensions, unfair sackings and employment tribunal claims by harmed whistleblowers.
Seven years on from Francis’ review, we see yet another scandal about poor care and whistleblower reprisal making its way into the mainstream media – the situation at University Hospitals Birmingham Trust, which has been the subject of two lengthy articles on BBC Newsnight.
Francis was not interviewed by Newsnight, but two individuals who have been party to his project were interviewed last night:
Philip Dunne
Tory MP for Ludlow, Health Minister 2016-2018, member of the Privy Council since 2019 and non executive director for Reaction Engines Ltd, for which he receives £3,400 monthly for eight hours work.
As Health Minister he was an enthusiastic promoter of the Freedom To Speak Up project, appearing at National Guardian’s conference sporting a lanyard.
Last year Dunne was criticised for calling for more military spending without declaring a £425 an hour job at aerospace company.
Helene Donnelly
A nurse who worked at Mid Staffs, reported that she was bullied for raising concerns and gave a statement to the related public inquiry about poor care. She described how records were falsified about A&E target times, including an admission that she went along with some of this, for in her opinion, justifiable reasons:

Donnelly took up a job as an Ambassador for Cultural Change at Midlands Partnership NHS Trust, and it was on this then unevaluated role that the whole National Freedom To Speak Up project was purportedly based.
There is a possibility that the model was in fact based on earlier arrangements in the civil service.
Donnelly has worked with the National Guardian to produce publicity material for Health Education England on Freedom To Speak Up and has blogged for the National Guardian:
U is for Understanding and Uniting
Donnelly has most recently left the NHS and is now reportedly Head of Safety Culture at the Nuffield Trust. I could find no details about this on the Trust’s website.
The BBC Newsnight interview 2 December 2022
I could not clearly hear the whole interview but neither Dunne nor Donnelly seemed willing to acknowledge the flaws of the Freedom To Speak Up model.
When Donnelly was asked about issues of independence, and whether Guardians should be people who have worked for an NHS trust, she stated in response that the responsibility for resolving issues lay with senior managers and not Guardians.
This response did not acknowledge that it was by policy, part of a Guardian’s duty is to escalate matters outside of a trust if the trust is failing to deal with concerns.
Hardly any Guardians do so of course, because they are trust employees and subordinates of the trust directors who they are implausibly supposed to hold to account. And people have families and mortgages.
Therein lies the core unworkability of the Freedom To Speak Up model.
Donnelly spoke about the “right” people being appointed as Freedom To Speak Up Guardians. The flaw of this narrative is that in a bad organisation, directors will appoint either bad apples like themselves, or they will ignore or even harm Guardians. The latter has happened on occasion.
Selecting the “right” people to be Guardians is immaterial in the worst organisations. In a bad organisation, the Freedom To Speak Up model is a recipe for either creating more victims of reprisal – the Guardians – or producing PR material to hide executive misconduct.
Dunne stated that the model works in “the best” NHS trusts. In the process he accidentally indicted his government’s handiwork. He implicitly acknowledged that Freedom To Speak Up does not work in bad trusts and that it is therefore ineffective. Moreover, as the model is unnecessary in trusts with good culture, it is a humongous waste.
Dunne muddied the waters by claiming that Freedom To Speak Up Guardians had not been in place for long in all places. This is strictly true of NHS quangos but the core objective of appointing Guardians in all NHS trusts was achieved about five years ago. So there is no excuse for the model’s failures on grounds that it is recent.
When Dunne was asked if performance targets could be counterproductive, he replied that targets were necessary so that staff could plan their rotas. Hmm.
Donnelly was critical of targets and argued that there should be more realism about what could be achieved.
Neither spoke about the underfunding of the NHS, which is at the heart of so many cover ups, although Donnelly in fairness did touch on understaffing.
I have transcribed the interview and reproduce it below.
One hopes that Newsnight will look further into these matters.
We are almost a decade on from the publication of the Mid Staffs public inquiry, which recommended that criminal penalties should be introduced for whistleblower suppression.
The government rejected this recommendation, and Francis did not later fight for it in his report of the Freedom To Speak Up review.
In fact, Francis seemed faintly derisive in his report of contributors to his 2015 review who asked for criminal penalties to be introduced.
If the media does not explore and report in sufficient depth the legal and political factors that drive continuing whistleblower reprisal and cover ups, we will likely be no further forward in ten years’ time.
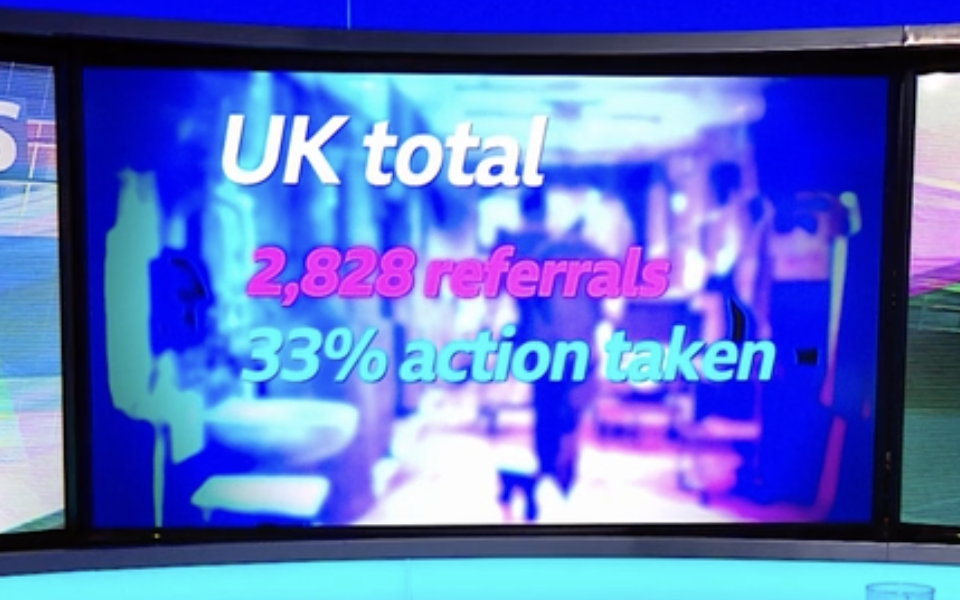
| The BBC have fallen on the fact that 26 GMC referrals over a ten year period by University Birmingham Hospitals resulted in no action against the referred doctors. The GMC advised the BBC that in contrast, nationally, 33% of referrals result in action. I sent the FOI data about UHB’s zero rate to UHB’s Freedom to Speak Up Guardian in June this year. I wonder what trust changes, if any, resulted from that. From: Minh Alexander <REDACTED > Subject: Outcome of GMC referrals by UHB Date: 18 June 2022 at 15:55:22 BST To: Julian Bion <REDACTED> Dear Professor Bion I write to pass on information that may be of interest to you in your role as UHB Freedom To Speak Up Guardian: https://minhalexander.com/wp-content/uploads/2022/05/uhb-referrals-to-the-general-medical-council-foi-2141.pdf This shows that 26 GMC referrals by the trust, 25 of which had medical director sign off, resulted in no further action by the GMC. I wonder if this makes UHB an outlier, as employer referrals to the GMC usually have a much higher likelihood of resulting in GMC investigation. I have also seen it said that employer referrals are more likely to result in GMC sanction, but I cannot find a supporting reference for this. Best wishes, Dr Minh Alexander |

MY TRANSCRIPT OF THE BBC NEWSNIGHT INTERVIEW 2 DECEMBER 2022 WITH DUNN AND DONNELLY
Kirsty Wark: So when a trust is deemed one step away from Inadequate as is the case for the Birmingham University Trust, facing so many allegations, how do you turn it round and change the culture?
We can speak now to Conservative MP and former Health Minister Philip Dunne and also to Helene Donnelly registered nurse and key witness in the Mid Staffordshire NHS Foundation Inquiry. More recently she’s been an ambassador for cultural change in an NHS trust. She’s now Head of Safety Culture at Nuffield Health.
Good evening both of you. This is really a question for both of you. There was a system established As we’ve just been hearing that was meant to improve culture after 2016, after the Mid Staffs inquiry.
Tell me first of all Philip Dunne why hasn’t that worked out the best it could?
Philip Dunne: So good evening Kirsty So I was in post following Sir Robert Francis’ report in 2015 and we introduced when I was a minister in the Department of Health the National Guardian system.
Which began in 2016 by the appointment of Dr Henrietta Hughes who stepped down only last year and she’d gone on to become the patient safety commissioner.
That has recruited a network of Freedom To Speak Up Guardians right across the NHS. I believe there are now 800 Guardians who are there to act as a first point of referral when people have got a concern or a complaint and last year there were over 20,000 cases reported through to these Guardians. They haven’t been in post in all settings for that long. I understand that from the last Freedom To Speak Up Index, taking a look at the questions asked in the annual NHS staff survey, that something approaching two thirds – I think it’s 65.6% of staff said in answer to the question they felt safe to report concerns. Now, I think that is good but clearly it means that there are another one third of trusts where they, staff don’t feel that. And that’s where the focus needs to be.
Kirsty Wark: Well Helene I wonder because you know all about the Guardians obviously. So is there an issue with who appoints the Guardians. Are they truly independent. And also do people know how to find Guardians? Do they even know that system existed?
Helene Donnelly: Yes there’s a huge amount of advice and guidance that comes through from the National Guardian’s Office. However they are limited because they are under resourced themselves and they don’t have any actual statutory powers [inaudible] ….trusts themselves really….[inaudible] who they’re appointing and how they’re appopinting them and ensuring they have the right people. There are requirements for them to be trained by the National Guardian’s Office and also should be registered with the National Guardian’s Office….[inaudible] but there are here some in posts associated with that. I think there does need to be more on national scale, a national conversation about what why these failings keep happening. Why there’s no accountability? And every time where there isn’t accountability it leads to further corrosion of trust for the public, for the workforce and we’re already seeing workers leaving the NHS.
Kirsty Wark: Just hearing Sharan talking about the fact that as she was raising concerns, as somebody that was nothing to do with the medical profession, the nurse was keying [?] into a computer what was going on but the nurse felt she couldn’t raise concerns. Clearly her father didn’t have cancer, he’d been treated for cancer and he knew his gallbladder had to come out [?]. That’s so incredibly shocking isn’t it? And it must give pause to people who think I’m not sure things are going right in my own case. People have to have trust in the system, and I wonder in some instances, do you think it should ever be the case that a Guardian should ever have worked at that hospital?
Helene Donnelly: I think erm that there are Guardians that have worked at the hospital but they are limited… [inaudible] ….they have to escalate the concerns to the senior leadership and the responsibility is on the senior leadership, not the Guardians to resolve the concerns.
Kirsty Wark: Let me ask Philip Dunne that. Because the trust has told us that they take patient safety very seriously, high reporting culture, rigorous investigation of patient complaint., But of course the Guardians can only as Helene was saying can only go so far They’ve taken to senior management but and of course senior management are under pressure with the targets and so forth, and clearly something is going wrong at the Birmingham Trust and indeed probably at other hospitals [inaudible] Birmingham trust.
Philip Dunne: So when I was in post, when I visited trusts that were in special measures I always insisted on meeting the senior Guardian within the trust and would ask them whether they had direct access to the chief executive or one of the non executive directors of the trust appointed to have that relationship. And I think that’s what’s essential – for the Guardian to be taken seriously they have to be able to escalate issues right to the top of the organisation. And then the chief executive or the non executive, they’re charged to do it, need to have the confidence of the Guardians when they’re taking cases to them that they will get investigated. That happens in the best trusts and should happen…
Kirsty Wark: Sorry to interrupt. What I was going to say was in our investigations in this hospital, there are allegations that there is mafia style management, and that the mafia style management is allegedly using the threat of the GMC and other threats to silence doctors who want to speak out. How concerned are you about that Philip Dunne?
Philip Dunne: Well I can’t talk about those allegations….
Kirsty Wark: No, not about those specific allegations
Philip Dunne: Well what I do say is absolutely right is that that the culture within the organisation needs to be one where we learn from mistakes. Mistakes happen. There are 1.5, one and half million patient interactions every day in the NHS. That’s 550 million in a year so things can go wrong. And when they do go wrong, we have to have a culture where we learn from our mistakes. That’s what the whole patient safety culture we’re trying to instil across the NHS is all about.
Kirsty Wark: Helene do you think excessive targets and different indices for outcome are actually counterproductive at the moment?
Helene Donnelly: Yes I do. And we saw this ten years ago at Mid Staffs. Even worse now given the current pressures and the knock on effects of that. The fact that I’ve got so many healthcare professionals striking, so many healthcare professionals leaving, it’s just adding more and more pressure and it’s not actually protecting patients more. We need to be more realistic about what can be achieved. We need to listen to our staff, to value the staff. If we keep losing valued and talented, experienced [inaudible] professionals throughout the health and social care system then we will not be able to care fpr patients. We need to value the workforce and listen to them when they speak up to raise concerns.
Kirsty Wark: The phrase that was used earlier was a phrase that the staff, the nursing staff, are sometimes just too tired to have time to care.
Helene Donnelly: Yeah I absolutely recognise that. I think there’s a huge degree of apathy that’s creeping in as well. I believe it’s worse than when I was experiencing the issues at Mid Staffs. I think staff are being actively discouraged from speaking up because of the pressures across the country. This isn’t obviously just about Birmingham. There are widespread issues. Of course we understand that, but we are seeing a workforce which is on its knees and it is undervalued and under supported and that leaves the staff not being able to care for patients as they should and it leads to absolute corrosion of trust from the public and from the workforce itself.
Kirsty Wark: So Philip Dunne, I wonder if you concur that targets and the pressures that they’re bringing on at the moment, are not fit for purpose?
Philip Dunne: Well I think targets to recruit more people into the clinical workforce are absolutely right and the government is on its way to meeting the targets that have been set for this parliament. I think since 2010 there are thirty four thousand more doctors working in the NHS and forty four thousand more nurses. So the workforce is growing. I think the fact that there are over twenty thousand cases reported last year of this issue, to the Guardians, suggests that something is going better than it was when there were none before this system existed. But I absolutely recognise there are very significant pressures on everybody working in the NHS at the moment. If we…
Kirsty Wark: But on that question….
Philip Dunne: Going on strike is not going to help
Kirsty Wark: On that question of the pressure I’m seeing, it’s not the targets for recruitment I’m talking about. It’s targets about getting a certain amount of care done by a certain day, a certain degree to day a certain amount of operations through the system. Sometimes that’s actually probably counterproductive and leads to more pressure. I wonder if you recognise that?
Philip Dunne: Well there’s an enormous backlog of cases that have got to be treated so I think trying to set some kind of guidelines about how many cases should be dealt with and by particular specialties, it helps people to plan their rotas. Surgeons have to have rotas.
Kirsty Wark: Let me ask you about that Helene. You think surgeons can organise their rotas and nurses will be able to work as hard as they could without targets to drive them on.
Helene Donnelly: Absolutely and the bottom line is that there isn’t enough. I can see there have been improvements in the last year, last few years but equally in that time, the population rises, the pressures on the workforce [inaudible] …lots of medics, lots of nurses and other professionals are retiring early. We’re recruiting more, so perhaps you know they’re lacking in expertise and clinical experience. We’re lacking that.
Kirsty Wark: Thank you both very much indeed.

A National Guardian newsletter featured this:

UPDATE 12 DECEMBER 2022
A BBC Newsnight interview with the UHB Freedom To Speak Up Guardian on 9 December 2022 raised further concerns:
What the UHB Freedom To Speak Up Guardian told the BBC
UPDATE 16 DECEMBER 2022
I have come across data which suggests that a UHB FOI disclosure of April 2022 about the outcomes of trust GMC referrals was incorrect.
I have written to the interim Chair Yve Buckland requesting clarification.
Letter to Yve Buckland UHB interim Chair 16 December 2022
PETITION
Please click and add your signature to this petition to reform UK whistleblowing law – whistleblowers protect us all but weak UK law leaves them wholly exposed, lets abusers off the hook and it is a threat to public safety.
Replace weak UK whistleblowing law and protect whistleblowers and the public
RELATED ITEMS
National Guardian’s gaslighting exclusion criteria: the never ending story
The National Guardian’s Office does not put a blue light on for ambulance staff.
Staff suicides at West Midlands Ambulance Service NHS Foundation Trust
The Disinterested National Guardian & Robert Francis’ Unworkable Freedom To Speak Up Project



I don’t wish to be flippant in responding to a most serious matter, but I can’t help wondering – if Father Christmas gifts me a sparkling new lanyard, would I be qualified to acquire a really prestigious job and read out lawyer-vetted, uplifting statements?
LikeLike