By Dr Minh Alexander retired consultant psychiatrist 16 May 2022
| Summary: The NHS trust which employed a bogus doctor Zholia Alemi as a consultant psychiatrist also allowed an unqualified healthcare assistant Samantha Robinson to practice far outside her scope for years as a specialist epilepsy ‘nurse’, running clinics and advising on specialist medication without any input from specialist doctors, sometimes for years. This was despite the situation being known to qualified clinicians and trust managers. When Jane Archibald a specialist nurse joined the trust, she was horrified to discover the situation. Her whistleblowing about this matter and other issues of concern was not met with a safe response by the trust. She experienced reprisal and an Employment Tribunal ultimately found that she had been unfairly constructively dismissed. A poorly executed grievance process was found to be a whistleblowing detriment, with a trust manager falsely claiming to the grievance investigator that the records of the whistleblowing disclosures were not available for inspection. The trust denied that Jane Archibald had made protected disclosures, right up to the last minute until the Tribunal ruled that she had. A disclosure letter that she sent to Stephen Eames the trust Chief Executive asking for his help with the unresolved patient safety concerns and her experience of reprisal was met only with silence. The Care Quality Commission was equally unhelpful and reportedly told her that the issues were an internal matter for the trust. Many issues remain to be resolved. |
On 13 May 2022 the Employment Tribunal published a most shocking judgment in the case of Jane Archibald, an unfairly sacked whistleblower. This is the judgment against North Cumbria Integrated Care NHS Foundation Trust, which sacked her:
The Tribunal determined that she had been unfairly constructively dismissed and that the poor handling of a grievance by her constituted a whistleblowing detriment:
“The complaints of protected disclosure detriment in relation to the complaints about the outcome of the grievance and the grievance appeal are well founded.”
Jane Archibald’s whistleblowing concerns and the trust’s poor response
Jane Archibald worked at Cumbria Partnership NHS Foundation Trust, a mixed mental health trust, between 2015 and 2020 as a Senior Nurse Practitioner/Specialist Epilepsy Nurse.
In her time at the trust, she discovered extraordinarily poor clinical practice.
The most striking discovery was that an unqualified healthcare assistant Samantha Robinson had been allowed to work for years without adequate supervision. She ran epilepsy clinics and advised general practitioners on specialist medication. Sometimes the patients were not seen by a specialist doctor, a neurologist, for years.
Epilepsy medication is powerful and sometimes toxic, and it is of great concern that an unqualified person was in a position to make changes to patients’ medication.
| Example This extract from the Employment Tribunal judgment gives the type of disclosure made by Jane Archibald via the trust incident reporting procedure, and the management response to the report: “Patient attended the Epilepsy Nurse Clinic for review at Hilltop Heights. Noted from the EMIS notes patient had not been reviewed by a Neurologist since attending the Neurology Department, patient transferred in November 2011. “Only person to have reviewed patient was SR Epilepsy Advisor. “SR [Samantha Robinson] had made reference to patient’s medication that she would make “no changes to patient’s medications”. “No evidence of a referral letter on transfer letter in 2011”. 33. Jonathan Kenworthy inserted in the outcome details: “SIRI investigation has identified the root cause of the incident – many lessons learnt including Sam Robinson no longer employed as Epilepsy Advisor. A lack of supervision and governance was historically cause of the issues. Investigation has resulted in epilepsy safety plan with clear guidance of appropriate service governance that is underwritten by Registered practitioners working with the patient group”. |
Robinson was referred to by some as a “neurology specialist” and or “epilepsy nurse”, as noted by the Tribunal, who also noted the trust management’s denial of the extent of the governance failures:
“24. In or around February 2015, soon after the claimant started her role, the claimant had a meeting with Samantha Robinson. Samantha Robinson told her that she had her own clinics. We find that she told the claimant that she prescribed medicines. Fiona Dixon [Senior Network Manager for the Neurology Service] did not think that an investigation found that she had done that; however, the document at page 217 indicates that she made recommendations about medication.
25.The claimant also discovered that Samantha Robinson was described on correspondence as a nurse. An example of this is at page 217. Samantha Robinson was not a registered nurse. There are various references in documents to Samantha Robinson as a “Neurology Specialist” (p.216), and “Epilepsy Nurse” (pp.224, 226).
26. We consider it more likely than not that Samantha Robinson described herself in this way with the knowledge of at least some managers and clinicians. This appears to be supported by the evidence of Fiona Dixon, who describes the concerns the claimant raised about Samantha Robinson being the “product of the historic structure” and why there was no disciplinary action against Samantha Robinson (para 25).”
One of Jane Archibald’s peers had reportedly supervised Samantha Robinson:
“21. It appears that Graham Bickerstaff may, at some time prior to the claimant’s appointment, have had some supervisory responsibility for Samantha Robinson. In her letter to the Chief Executive dated 8 August 2019 (p.559), the claimant wrote that she had been told by Graham Bickerstaff that he used to be her supervisor. The claimant, in submissions, also relied on the document at page 763, on which Graham Bickerstaff is described as Team Leader, of the neuroscience service”.
Very worryingly, Robinson saw many vulnerable patients with a Learning Disability. She also saw patients who were women of child bearing age, with regards to the teratogenic effects of some anti-convulsant medication, especially sodium valproate. The latter can cause devastating harm to developing babies in the womb, resulting in major congenital malformations, developmental delay, intellectual disability, neurological and psychiatric disorders:
Foetal Valproate Spectrum Disorder
When Jane Archibald raised concerns about this surreal situation, she was met with an equally surreal organisational response. According to Archibald, no rigorous investigation was mounted and those responsible for allowing this situation oversaw the organisational response to her concerns.
The Employment Tribunal noted that Fiona Dixon the Senior Network Manager for Neurology suggested in incident forms that Samantha Robinson was removed from her post for malpractice. But the Tribunal found that the reality was that Robinson went off sick and was simply allowed to leave the trust via redundancy. An astonishing failure of Safeguarding:
“28. Samantha Robinson went on sick leave and remained on sick leave until she left the trust. Her employment was terminated by reason of redundancy and no disciplinary action was taken against her. We consider that this is contrary to the impression given on incident forms, which suggest she was removed from post because of concerns about her practice e.g. as referred to in the incident form completed 21 December 2015 on which Fiona Dixon wrote: “The unregistered member of staff was investigated and is no longer with the Trust.”
This saga of Samantha Robinson being allowed to masquerade as an epilepsy specialist is all the more concerning because Cumbria Partnership NHS Trust is where the bogus doctor Zholia Alemi, who posed as a psychiatrist for years. This first came to light through the diligent investigation of a local press reporter.
Doctor who faked will of west Cumbrian widow led life of deception
Jane Archibald also found serious problems with the use of buccal midazolam for epilepsy by nurses, mainly within the Learning Disability section of the trust. This drug is a sedative and can cause respiratory arrest. Archibald found that midazolam was not used within protocol, placing patients at risk, and that some nurses acted outside of their remit.
Reprisal and lack of protection
As a result of raising concerns, Jane Archibald found herself increasingly ostracised.
Managers started focussing on the manner in which she raised concerns, rather than the concerns. They asserted that her communication style was poor, when audit information indicated no such communication problem. It was also despite the fact that Jane Archibald’s record was hitherto unblemished. As the Employment Tribunal noted, although trust managers criticised Archibald’s communication style, they did not actually offer her any help or training with the alleged issue. When her immediate colleagues were hostile or unsupportive, managers suggested that it was her manner of raising concerns that caused problems.
One manager even suggested that the alleged communication problems were due to Jane Archibald’s diagnosis of epilepsy (which had been well controlled):
“135. On 7 June 2019, Fiona Dixon was interviewed in the grievance investigation. The interview included Fiona Dixon saying: “I have no concerns of her clinical knowledge but the impact of not being able to communicate with MDT and patients it then gets fractured, I do feel sorry for her because it is not deliberate, I think it may be linked with her epilepsy but how do you raise that?”
It was a particular disappointment to Jane Archibald that the Tribunal made no finding of discrimination on this point.
There was even a complaint which related to Archibald wearing a cardigan and refusing to take it off because she was cold. Many whistleblowers will relate to this type of ridiculous non-complaint, that arise when employers struggle to find dirt on conscientious, competent employees.
As a well-controlled epilepsy sufferer herself, Archibald’s health began to deteriorate. After eighteen years symptom free, she began experiencing breakthrough symptoms again.
Jane Archibald wrote to the then trust Chief Executive Stephen Eames in August 2019. At that point, Cumbria Partnership was in the process of merging with North Cumbria to create the current North Cumbria Integrated Care NHS Foundation Trust. The merger was completed in October 2019.
In the letter to Eames which I have seen, Archibald very clearly set out the history of her concerns and difficulties at the trust, especially her shock at the trust’s response to the issue of an unqualified healthcare assistant working as a senior specialist nurse.
Archibald reports that she did not even receive the courtesy of a response from Eames. This was cited in Tribunal proceedings and not disputed by the trust.
“147. On 8 August 2019, the claimant wrote to the Chief Executive of the respondent Trust. She wrote that she was writing to highlight concerns which she believed were in the public interest. She wrote about concerns she raised about Samantha Robinson working outside her scope of practice and about lodging other incidents regarding controlled medication, most of which involved Learning Disability Nurses, who she found to be working outside their scope of practice…. The claimant received no response to her letter to the Chief Executive.”
This is not the first time that a concern has arisen regarding Stephen Eames’ interaction with a whistleblower. On this I will provide more at another time.
| Stephen Eames Stephen Eames has held many management posts in the NHS. This is a copy of his LinkedIn entry as of 14 May 2022. This is a most detailed and harrowing account by UNISON of the grievous impact on staffing, beds and services caused by a PFI financial black hole at Mid Yorkshire Hospitals NHS Trust, where Stephen Eames was CEO from 2012 to 2016, and reportedly received a salary of approximately £300K: Deadweight Most recently, he has been appointed as Chief Executive of the Integrated Care System in the Humber region. He was Chief Executive of the Mid Yorkshire Hospitals NHS Trust between 2012 and April 2016 when the trust’s handling of whistleblower cases gave cause for concern. One of these cases was that of Gillian Wright a manager in the trust Occupational Health Department who raised concerns from 2013-2015 about corrupt practices of nepotism, fraud, breach of the Medicines Act and covert monitoring of her email. Gillian Wright experienced reprisal after raising concerns and later sued the trust. The Employment Tribunal found that she had been unfairly constructively dismissed and that the trust subjected her to whistleblowing detriment by claiming that she “ might be the problem in her relations with three of her interim managers.” This obviously has similarities with Jane Archibald’s case. This is the Employment Tribunal judgment in Gillian Wright’s favour against Mid Yorkshire Hospitals NHS Trust: ET Judgment Gillian Wright v Mid Yorkshire Hospitals NHS Trust Case Number 1801081/16 Eames calls himself “Professor”. This appears to be on the basis of an honorary title from the University of Central Lancashire (UCLan): North Cumbrian NHS chief Stephen Eames becomes Honorary Professor at University of Central Lancashire. This puts him in good company with the disgraced Paula Vasco-Knight who used to call herself “Doctor” based on an honorary doctorate. Like Vasco-Knight, Eames was also given a CBE Professor Stephen Eames awarded CBE in Queen’s Birthday Honours I will provide more information about another whistleblowing matter at Mid Yorkshire Hospitals NHS Trust in due course. |

Instead, the usual dreadful NHS whistleblower playbook rolled on. Jane Archibald was isolated and vilified. Her grievance about mistreatment was extraordinarily poorly handled and the grievance report joined the chorus about her alleged communication problems, despite Archibald’s previously unblemished record.
Moreover, Jane Archibald was later offered support from a Freedom To Speak Up Guardian who had given evidence against her during the grievance investigation.
| The trust’s compromised Freedom To Speak Up process According to the Employment Tribunal, Linda Turner Quality and Safety Lead gave hearsay evidence against Jane Archibald to the grievance investigation: “133. Fiona Dixon suggested Martin Daley [the grievance investigator] should speak to Linda Turner. Linda Turner said that she personally had never had an issue with the claimant but a lot of people had told her that they had less than positive experiences of working alongside the claimant. Linda Turner said that a lot of the claimant’s concerns were based on clinical evidence and some of the things she had raised had been brilliant and led to improvements being made. She said the claimant appeared to struggle with email communication and she was aware that other clinicians had been upset by the tone and content of some emails the claimant had sent. She said that the claimant had raised a number of incidents and it was positive that she had picked up on service gaps in development and training. The notes record: “She concluded that Jane has demonstrated some good work and identified issues well but that the main concerns noted come back to communication and people feeling that she doesn’t value them or doesn’t recognize their skills.” The Tribunal noted that in December 2019 the trust offered Jane Archibald the option of support from Linda Turner in her capacity as Freedom To Speak Up Guardian, but she understandably declined this. “She was invited to speak to the Freedom to Speak Up Guardian, Linda Turner, but refused to do so.” |
The Tribunal concluded that Jackie Molyneux Team Lead for Neurology, who was one of the subjects of the grievance, misled the grievance investigator:
“Martin Daley [the grievance investigator] asked Jacquie Molyneux whether there were copies of the incident forms. Jacquie Molyneux replied “we don’t keep a copy of the incidents”. When asked about this in cross examination, Jacquie Molyneux acknowledged that she could get the incident forms from the computer system. She did not volunteer this information to Martin Daley. No one subsequently corrected the misleading information given by Jacquie Molyneux to Martin Daley, so he did not obtain the relevant incident forms as part of his investigation.”
| The trust’s response to Jane Archibald’s grievance about whistleblower reprisal The grievance investigation into Jane Archibald’s concerns about her experience of whistleblower reprisal was fundamentally flawed because the investigator made no examination of her whistleblowing disclosures, which were mostly in the form of formal incident reports. There were also other procedural failures in the grievance investigation. The grievance instead focused on her colleagues’ allegations about her manner of communication. The Employment Tribunal determined that not only was the grievance procedure fundamentally unfair and a whistleblowing detriment, but that the subsequent grievance appeal process was also detrimental: “The appeal was not a rehearing. We conclude that it was, therefore, tainted by the original flaws in the grievance investigation. We conclude that the claimant was subjected to a detriment by receiving a grievance appeal outcome relying on a flawed grievance process.” |
Occupational Health advice to Archibald’s employer was not taken seriously. She went off sick, with stress exacerbating her epilepsy. She eventually resigned, without a job to go to, when it was clear to her that all hope of any fair resolution was gone. The detriment continued when the trust gave her an indefensibly poor reference for a new job with another organisation. This was later criticised by the Tribunal and recognised as a detriment.
Her claims to the Employment Tribunal were partially upheld. Remarkably, the Tribunal accepted that she had suffered whistleblower detriment, a rare finding. It also agreed that she had been unfairly and constructively dismissed.
One of the most egregious aspects of the case is that right up to the end, North Cumbria Integrated Care NHS Foundation Trust refused to accept that Jane Archibald was a whistleblower. Despite her many, serious protected disclosures.
Farcically, the trust argued during Tribunal proceedings that her disclosures were not protected because they were just part of her job:
“219. The respondent also suggested that the claimant was not making protected disclosures because she was raising matters as part of her day to day job.”
The Tribunal gave this short shrift and determined that Jane Archibald had made serious protected disclosures.
“We conclude that it does not matter that it was part of her job to flag up such concerns and complete incident forms where appropriate; the statutory test does not prevent concerns raised as part of a person’s day to day job satisfying the statutory test for protected disclosures.”
“….the incident forms we have seen which all raise legitimate concerns, most of a serious nature.”
Damningly for the trust and reflecting very badly on its persistent denial, the Tribunal accepted all of Archibald’s pleaded disclosures as protected disclosures:
“221. We conclude that all the disclosures relied upon were protected disclosures.”
But the trust has inadvertently impaled itself on a sharpened stake of its own making: it has publicly recognised that Jane Archibald was being a professional and just doing her job in raising concerns.
Small vindication though for all the suffering and lost years.
Regulators and the governance aftermath
Jane Archibald raised concerns with the Care Quality Commission but was told it was an internal matter for the trust.
The correspondence is no longer available as she sent the email from work and she does not have access to it.
| The Care Quality Commission and North Cumbria The Care Quality Commission has a deeply worrying history of helping to minimise patient safety problems at North Cumbria University Hospitals NHS Trust, a predecessor body of North Cumbria Integrated Care NHS Foundation Trust. North Cumbria University Hospitals NHS Trust which was one of the fourteen “Keogh” trusts with high death rates. This is a risk summit summary from 2013 in relation to difficulties identified at North Cumbria: North Cumbria University Hospitals NHS Trust Risk Summit report July 2013 A later FOI response from the CQC showed that the CQC reacted reluctantly to numerous North Cumbria whistleblowers’ disclosures, often effectively just putting even the most serious disclosures in a drawer. The FOI material can be found in this report: Whistleblowers unheard by CQC |
Many questions remain from this unedifying tale. The trust can clearly not be trusted to put right the mess of the unqualified healthcare assistant unsafely treating patients for years. Neither can the CQC it seems. Much more rigorous scrutiny is needed. In the first instance, I have asked NHS England/ Improvement to look into the matter and to review Stephen Eames’ role in particular with respect to his current post as Chief Executive of the ICS Humber, Coast and Vale Health and Care Partnership, copied to his Chair Sue Symington.
| Sue Symington Sue Symington is Stephen Eames’ boss as recently appointed Chair of Coast and Vale Health and Care Partnership. Symington was a non executive director at Harrogate and District NHS Foundation Trust until 2015 From 2015 she has been Chair at York Teaching Hospital NHS Foundation Trust. York Teaching Hospital NHS Foundation Trust unfairly constructively dismissed another whistleblower in 2019, Elaine Middleton. Elaine Middleton was a senior psychologist. who raised concerns about the trust adopting a cheaper model of staff support for staff coping with traumatic events at work, against NICE guidelines for trauma. I asked York about its learning from this matter. York Teaching Hospital NHS Foundation Trust CEO’s response of 18 March 2022 was not overly remorseful in tone: “Dear Dr Alexander, Thank you for your email. As with any Employment Tribunal outcome we gain learning from the judgement. The learning from the judgement is used to improve our systems and processes. This was the case for the Tribunal you reference below. The Tribunal clarified for us the need for the Trust to ensure the accuracy of job descriptions and this has now been implemented. I feel it helpful to clarify that the tribunal confirmed the whistleblowing concern was handled appropriately and there was no connection between that and the dismissal. Kind Regards Simon Simon Morritt Chief Executive” |
I have raised concerns with Sean O’Kelly the new CQC Chief Inspector of Hospitals about the local CQC inspection team’s response to Jane Archibald’s disclosures. I have asked him to ensure that CQC reviews the trust’s compliance with regulations, especially Duty of Candour to all the patients and families affected by the trust’s negligent failure to supervise Samantha Robinson properly.
I have also asked the current trust Chief Executive Lyn Simpson for comments and information. One of the questions I have asked the trust is whether those responsible for supervising and managing Samantha Robinson have been investigated, disciplined or referred to the Nursing and Midwifery Council by the trust. I have also asked the trust for evidence of any trust Safeguarding actions arising from the Samantha Robinson matter. At the time of writing, no comments have been received.
Jane Archibald’s case is back in court for a remedy hearing on 15 July 2022 for anyone interested in attending and following up this remarkable case.
Whilst Jane Archibald was suffering whistleblower reprisal, the National Guardian’s Office was helping to legitimise and publicise the trust’s whistleblowing governance:
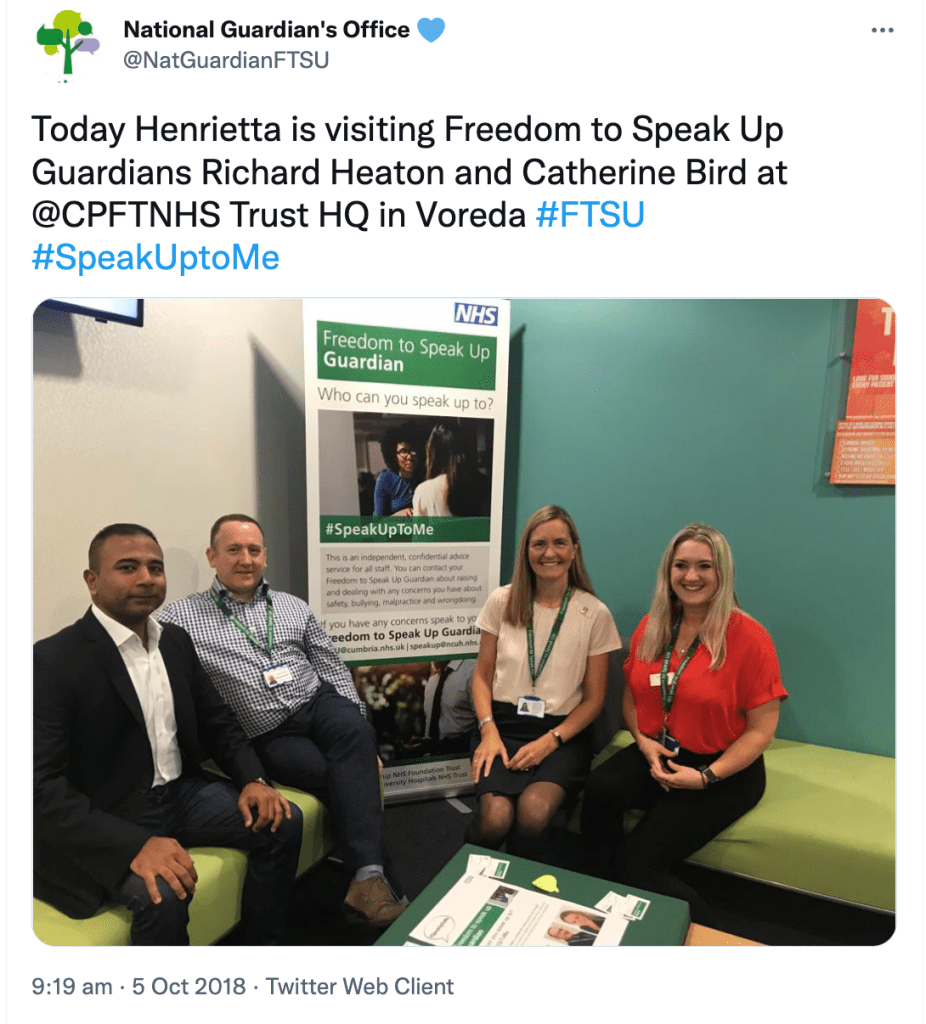
This is the trust Freedom To Speak Up Ambassador, who gave hearsay evidence against Jane Archibald, discussing the importance of giving staff confidence to speak up when things go wrong:
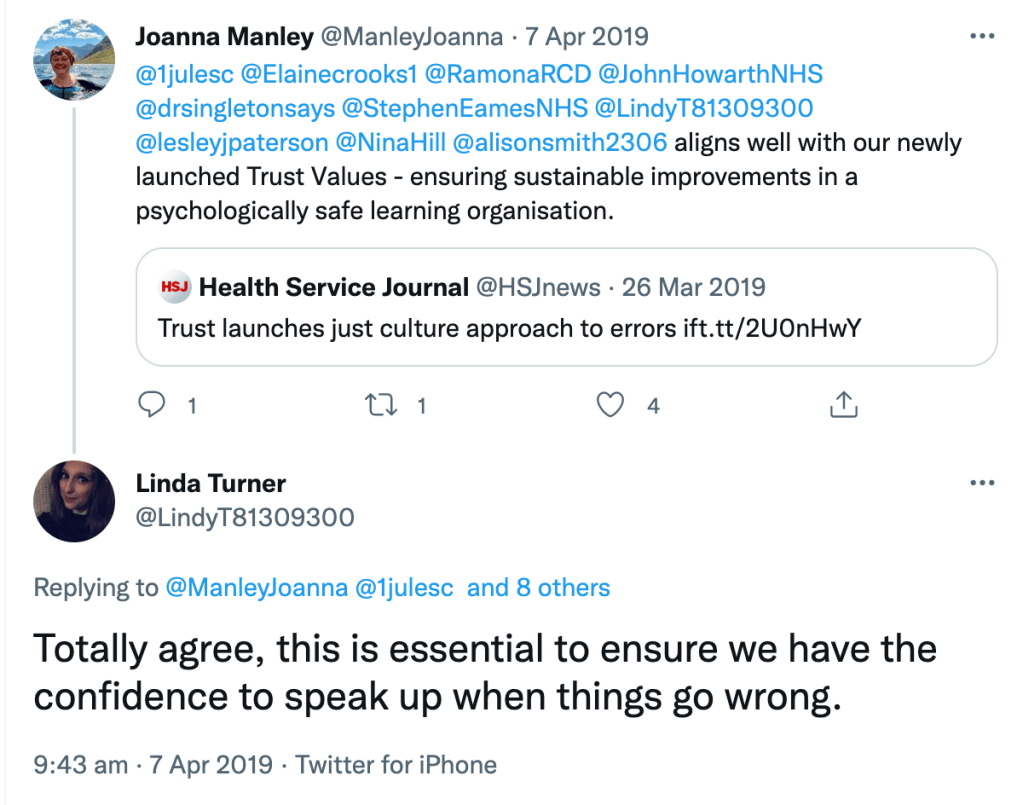



Dear Dr. Alexander,
I just read through the whole saga regards Ms. Archibald. I understand why you are working hard to strengthen whistleblower laws. Ms. Archibald’s did the right thing reporting her colleague and far too often in such cases the governance hierarchy turns on those raising legitimate concerns about patient safety. I think your follow up questions to those responsible and publishing all the associated findings, outcomes and unanswered questions would be most appreciated by Ms. Archibald. And of course everyone else depending on the NHS to receive safe, transparent, accountable, collaborative and quality care. I am learning a great deal from your blogs. I am certain many people appreciate and are benefitting from the work you do. I hope the new laws needed to protect whistleblowers and the public will happen sooner rather than later.
Kind regards.
James
LikeLiked by 1 person
Thank you, Dr A.
Let’s hope Jane Archibald has recovered from her appalling treatment within an unprofessional and obviously indifferent/incompetent system.
James expresses my thoughts (or those I can express without danger of arrest) – thank you, James.
It seems that nothing can penetrate the defences of the guilty parties. I am reduced to longing for the photographs of the smiling people to be printable. I would thus have the pleasure of inking in the teeth and adding suitable moustaches.
Hopefully, Jane Archibald is heartened to know that others are affronted by her treatment and that she obtains employment within a civilized and responsible organisation.
LikeLike
Jane archibald was an excellent and very knowledgeable epilepsy nurse, my son seen sam robinson and been only recently diagnosed at the time you just excpect to be seeing a professional specialist nurse as it says on the paperwork, at the time jane came along i noticed quiet quickly the stark difference between her professionalism and sams to the point that i asked her “how are you so knowledgeable on epilepsy she was amazing and telling you in a way you could understand and gave hope again” she said because im a specialist epilepsy nurse, to which i said wasnt the last one? Its a shame shes been forced to leave she was a lifeline for suffers and to think its brought her own symptoms back is beyond words she spoke up because she is a real nurse on and off the job dedicated, there to help and care for her paitiants and put there safty first, shame on the trust youve lost somone who will not be easily replaced, i hope jane gets back to a stable level with her own epilepsy and can find a way to still help other suffers she was unique kind caring and very very knowledgeable, we need more whistle blowers like her and cqc should of investigated So shame on them as well.
LikeLiked by 1 person