Governments intermittently make glib promises to lift neglected and under-funded mental health services out of second class status, but usually only disappoint in the end.
The health regulator the Care Quality Commission (CQC) is regarded as an unhelpful if not hostile force by the majority of whistleblowers, with concerns from whistleblowers about CQC politicisation, confidentiality, employer bias, active protection of abusers, wilful blindness and failures to respond appropriately to disclosures.
Despite a major investigation of West London Mental Health Trust in 2009 1 triggered by CQC’s predecessor the HealthCare Commission, which generated common sense recommendations for addressing safety problems in struggling mental health services, the CQC has not distinguished itself in championing the needs of mental health patients.
Headlines have continued about familiar, recurrent failures.
At Southern Health NHS Foundation Trust, CQC failed to detect or report gross failures in the handling of hundreds of deaths. 2 The Mazars deaths review on Southern Health NHS Foundation Trust found that CQC did not even have the right number of deaths of detained patients. Mazars also questioned the reliability of CQC’s intelligent monitoring data .
CQC has been insufficiently critical of excessive mental health bed closures even though a recommendation from the West London investigation was that adequate beds were needed for safety. When asked about CQC’s approach to regulating safe numbers of mental health beds, CQC’s deputy Chief Inspector said that CQC preferred to only regulate the effects of bed shortage. Not exactly proactive then. 3
I have kindly been sent FOI data on whistleblowing by mental health trust staff to the CQC, which shows over 700 whistleblower ‘enquiries’ over a four year period, 1 April 2013 to 1 March 2017:
CQC FOI disclosure 8 March 2017
The whistleblowing enquiries to CQC are likely to have been made by trust staff who could not progress their concerns within their own organisations, or for some other reason did not wish to make an internal disclosure.
Extrapolating from CQC’s data gives an overall average of 3 whistleblowing enquiries per mental health trust each year.
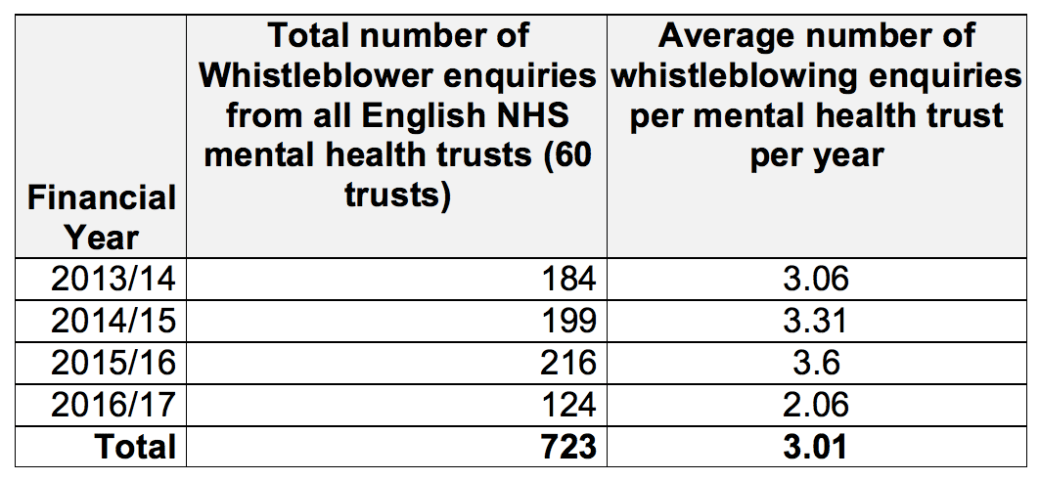
Curiously, there has been a sharp dip in the number of enquiries in the last financial year. CQC have denied any change in their recording method. IF that is so, a number of other possible factors could be responsible for the drop. However, it seems unlikely that staff have stopped disclosing because things are going well.
The mental health trust that has had the highest recorded number of whistleblowing enquiries to the CQC in the last four years is Norfolk and Suffolk NHS Foundation Trust, which CQC recently and controversially took out of special measures despite continuing concerns about safety and deaths, and continuing bed cuts.
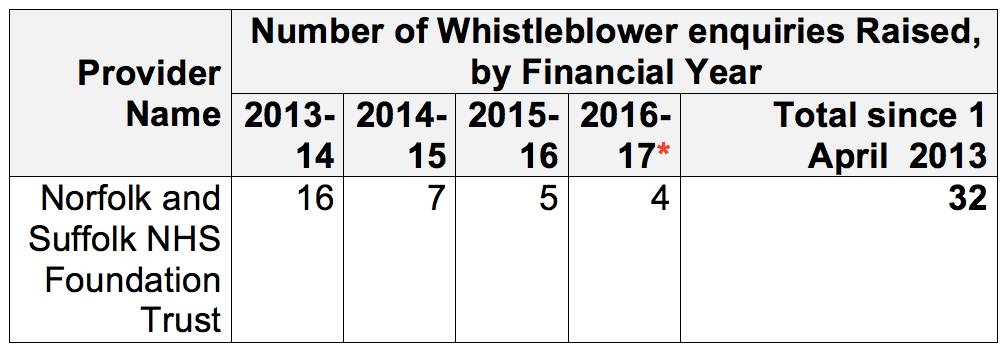
See the Norfolk and Suffolk Crisis campaign website for full details:
http://norfolksuffolkmentalhealthcrisis.org.uk/
HOWEVER, on this occasion the CQC has given an especially elaborate disclaimer about what its data actually means:
“We should advise you that the number of ‘whistleblowing’ enquiries recorded against each provider will not necessarily be representative of the actual number of whistleblowing concerns reported to us.
This is because an enquiry recorded as ‘whistleblowing’ may contain:
- A single concern from one whistleblower
- Multiple concerns from one whistleblower
- Multiple concerns from multiple whistleblower’s that are linked to a similar issues
- Multiple concerns from staff who have been invited to contact CQC with feedback ahead of an inspection where one enquiry is recorded as whistleblowing
- Positive and negative intelligence about a location and provider
- Information wrongly categorised as whistleblowing”
CQC’s claim that “whistleblowing enquiries” may contain positive feedback is implausible, or at best unrepresentative of the great majority of contacts, based on various disclosures that I have seen regarding specific trusts.
For example, in the same above FOI disclosure, specific whistleblowing data was given on two trusts with recent whistleblowing governance issues – North Essex Partnership NHS Foundation Trust and Berkshire Healthcare NHS Foundation Trust. No positive feedback is evident. Instead, there are concerns about safety, patients at risk of self harm, poor service, falsified documents poor incident recording, bullying, staffing, poor service, bed cuts, safeguarding, racism, and poor management of change:
CQC FOI DISCLOSURE NORTH ESSEX AND BERKSHIRE IAT 1617 0775
As for CQC’s obfuscation on the precise numbers of whistleblowers and concerns, the regulator should be recording whistleblowing data in a way that shines light on what is happening, not doing the dance of the seven veils.
Regarding the extraordinary comment by CQC that it might be incorrectly classifying some events as ‘whistleblowing’ when they are not, what can one say? An organisation that costs as much as two mental health trusts ought not to record data that is so inaccurate that it cannot be relied upon.
However, CQC’s purpose in contriving such looseness and ambiguity may be revealed by CQC’s assertion that its whistleblowing data “should not be used as an indicator of Trust performance”.
The Department of Health would surely be proud of such pliable, elastic data that could be made to mean whatever you want it to.
And despite a recent CQC attempt to spin that it is now more responsive to whistleblower disclosures 4 – following criticism at the end of last year 5 – please note that none of the 2016/17 disclosures for North Essex and Berkshire Healthcare resulted in inspections being brought forward.
But then, it’s all in the fancy footwork, how you do your sums and how much or how little you reveal.
UPDATE 25 APRIL 2017
If CQC carries on recoding whistleblowing data on the above basis, it will fall foul of new legal requirements for bodies that are ‘Prescribed Persons’ under the Public Interest Disclosure Act to publish the numbers of whistleblowing disclosures received and responses to the disclosures. These new legal requirements came into force at the beginning of this month. I have now written to the National Guardian about her employer’s shortcomings, copied to the relevant parliamentary committees.
Letter to Henrietta Hughes re CQC WB data 25.04.2017
RELATED ITEMS
https://minhalexander.com/2016/12/05/whistleblowers-unheard-by-cqc/
https://minhalexander.com/2016/12/15/covering-up-the-cover-ups-cqcs-revisionism/
https://minhalexander.com/2016/09/25/cqc-deaths-review-all-fur-coat/
REFERENCES
1 Report of Investigation into West London Mental Health Trust by the Healthcare Commission. CQC 2009
WLMHT HCC Investigation_into_West_London_Mental_Health_NHS_Trust_FINAL_200907171608
2 Mazars report of Independent review of deaths of people with a Learning Disability or Mental Health problem in contact with Southern Health NHS Foundation Trust April 2011 to March 2015, December 2015
https://www.england.nhs.uk/south/wp-content/uploads/sites/6/2015/12/mazars-rep.pdf
3 Email from Paul Lelliott 19 December 2014:
“I think therefore that the correct approach for the CQC to take is not to try to count bed numbers but to assess services for the ‘symptoms and signs’ of pressure on bed availability eg. problems with admitting a person who needs to be in hospital for their own wellbeing, people being admitted to a ward distant from their home, people being moved from ward to ward during an admission episode, people being discharged before they are ready etc.”
4 CQC Board Paper Feb 2017 CM021705_Item5_Q3performanceReport
CQC Health Service Journal April 2017 Insp brought forward after WB
5 Whistleblowers unheard by CQC. Alexander, Linton, Sardari and a fourth NHS whistleblower December 2016
https://minhalexander.com/2016/12/05/whistleblowers-unheard-by-cqc/


So much I want to say but wisely will not.
I shall thank you and I shall ponder the younger members of the Royal family wearing blue headbands to publicise and support Heads Together – the charity that suggests we all talk about mental health.
We might as well talk about it, because as I understand the situation, there is little funding or political attraction in actually addressing the issues surrounding such. In addition, it seems whistle-blowers will continue to be ignored unless they manage to slip the blue headbands down some inches and wear them around their mouths to indicate the true situation.
Thank you,
Zara.
LikeLiked by 1 person
Zara could not have said it better. The CQC is an utter and total joke. Mental health Trusts lie and cover up abuse and crimes because they can do so with impunity. They know that there is no real or serious oversight and they can basically get away with literally anything. The best advice I can give anyone is never ever have contact with these services. If you can’t avoid this than document and record all contact I guess.
LikeLiked by 1 person